jdeon
Before and After
Oct 28, 2011
My sleeve sister Tracy was in St. John's today for appointments so we got to see each other. She looks FANTASTIC and it was so good to see her.
Today is five months and seven days since our VSGs were done here at the Health Sciences Centre.
So we decided to take a picture together and used our driver's license pictures are our "before" pics:


Yeah, wow, eh? Even we were amazed at the difference.
So sweet - thank you God!
Back in the 100s
Oct 04, 2011
Yup - back in the 100s. Never thought I see it again!
Sold, donated and traded away most of my X clothing on the weekend. Mourning the loss of some beautiful clothes a bit, but moving on. Off to Toronto today for a little vacation/shopping trip as my reward. :)
Still feeling good - still challenged in learning how much and what is okay to eat, but learning bit by bit.
Working on kicking off a support group for NL Sleevers - pre-surgery and post-surgery - apparently there are now 10 of us who have now been done!
Not losing any hair, thank goodness - it might be thinning a bit, but not really noticable. I am grateful that I kept and will continue to keep up those protein shakes every day - protein is everything in this journey, I am realizing.
Happy Thanksgiving to y'all and don't let the turkeys get you down!
The low-down on the down low
Jul 28, 2011
So….now I can add blog guilt to the list. (Heck, I’m Catholic, so if there’s a new type of guilt out there, I’m all over it.) Sorry for not updating in the last many weeks.
Life resumed. With all of its busyness and deadlines and sleepy sunshine. Looking amazingly similar to my pre-surgery life, but there are distinct differences.
For instance, there are only so many hours I can go before being reminded about my post-bariatric surgery requirements and restrictions, which is very grounding.
No matter how busy I am, I have to pull back and keep my health as my priority by thinking about how much water I have consumed, what I should be eating next and when, and when I can work in time in my day for exercise.
Pre-surgery, I would get my day going with a traveler mug of coffee and a toasted bagel with some sort of cheese, both usually consumed in the car.
Post-surgery, I have to have a glass of water with some meds first thing when I wake up, because one of them is supposed to be consumed ½ hour before I eat. Then I have to start my day with a protein shake, which gives me 45-50 grams of my minimum 80 grams of protein I have to consume each day.
(Why so much protein? After bariatric surgery, you must take in sufficient protein every day to speed wound healing, preserve your lean body mass, enhance your fat-burning metabolism and minimize hair loss. For more, read this.)
Bagel? Forget about it – it would take me the entire day to each one. And thankfully, I don’t miss it at all.
Coffee? I had my first one a few days ago – a small Tim Hortons around 9:30am. Not bad. I sure had extra pep for the day. But it’s a slippery slope when it comes to caffeine, so I think I’ll still save it for the occasional use instead of making it a regular habit again.
(Why is caffeine bad after bariatric surgery? Weight loss surgery patients can hold only small amounts of fluids in their stomach pouches, so we have to sip water frequently throughout the day to prevent dehydration. Since caffeine has a diuretic effect, meaning that it causes water loss through excess urination, we have to be really careful. Dehydration also increases the risk of developing kidney stones after weight loss surgery. For more, read this.)
Exercise is just a difficult to make time for now as it was pre-surgery. The only difference is my motivation. Obviously there are some days I am still a schlump, but most days I am happy to say I have been making the time.
Thank God for the amazing nature trail next to my workplace – I either park at one end in the morning and walk in and back each day, or my husband meets me at lunch and we walk the whole thing together. All told it’s about 2 ½ miles of walking exercise each day – and I am secretly hoping to be able to start jogging/running in a few months.
Socializing is sometimes challenging for me post-surgery. Caught up in the good times being with good friends, occasionally I forget myself and try foods I shouldn’t or eat too fast. Then the good times get interrupted abruptly when I have to excuse myself to go and throw up.
Which is kind of a good thing. Sleevie (my new sleeved stomach) doesn’t brook any funny business. If it’s not good for Sleevie, or it’s too much for Sleevie, Sleevie sends it back. Which is an excellent reminder for me to get back on track tout de suite.
(But to my extreme joy, I have figured out that I can enjoy red wine again – again, moderation being the key, but Sleevie seems okay with it, as long as I balance out possible dehydration issues.)
Okay, now for the good news:
- I have already shed over 50 pounds and dropped three dress sizes (from 22 to 16).
- Hardly ANYTHING in my closet fits me anymore.
- I can handily walk/jog up the three flights of stairs at my work.
- I can cross my legs again.
- I can not only wear but also DANCE in high heels again.
- My blood pressure is excellent and my doctor will be taking me off those meds soon.
- My lungs and asthma have been in terrific shape in the last few weeks.
- My back and joint pain is almost non-existent.
- I look feel as hot as balls.
The challenges I am facing now are mostly with staying grounded and smart.
While I can’t imagine there ever coming a day that I forget that I had bariatric surgery, already there are moments, and that is when the danger occurs. Already I have dropped off journaling everything I eat, so I hope that my brain is calculating my intake properly.
I am relying more now on my instincts and how I am feeling to guide my eating and activity – I don’t know if that is okay, but I suppose the scale will tell the tale.
Today I am 219 pounds. I am still obese, but not morbidly so anymore. My hope is to be “just” overweight, which for me comes about 40 more pounds from now.
I might get there. I might not.
Anything I am is okay from here on out, as long as I am healthy.
NSV (non-scale victory)
Jun 16, 2011
I am wearing jeans today I haven't worn since my son was born!
Take THAT fat cells! Woot!
Riding the rapids three weeks post-op
Jun 09, 2011
Three weeks post-op
March 22: 270 lbs
May 20: 248 lbs
June 10: 235 lbs
(warning: the following post contains the wanton use of animated emoticons that may be offensive to some viewers)
I can’t believe it’s already been three weeks since my surgery! It’s gone so fast.
In the last 21 days, my weight has gone from 248 at my pre-admission to 235 as of this morning according to my oh-so-friendly Wii Board. Which is a little more than 2 pounds per day.
Obviously, I don’t expect this to continue at this rate forever, otherwise I would be a zygote by Halloween (ooh, costume idea). But it’s damn motivating right now!
My six laparascopic incision sites are healing terrifically. No pain at all to speak of past week one.
Here is what they looked like at 3 days post-op with the staples still in:
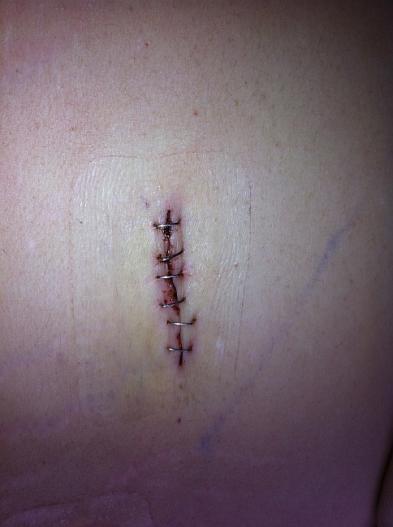
Here is what they look like 3 weeks post-op:
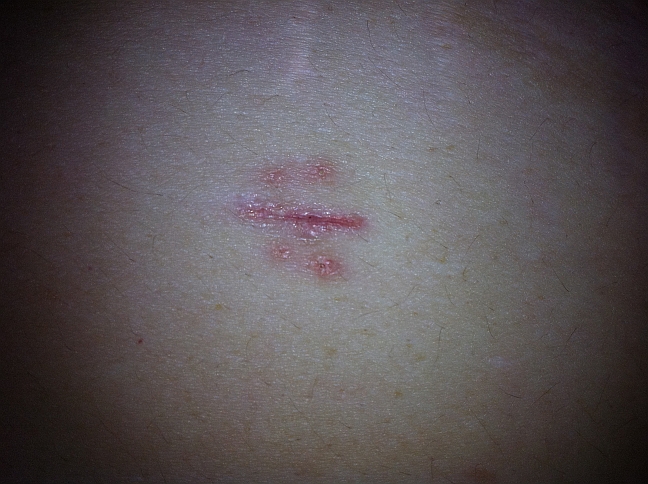
My diet and exercise is going well. As I am rebel with a cause, I am following these diet guidelines from Cornell University’s bariatric program, which are working well for me. Eastern Health is just getting their program up and running so I am looking forward to sharing my experiences so far with their newly-hired bariatric dietician next week.
I track my diet very carefully, which is easy thanks to technology. Basically I am consuming no more than 800 calories per day, which are mostly full liquids, with one mushy meal of about ¼ to ½ cup of something like mashed potatoes, scrambled egg, soft meatloaf or flaked fish per day.
The only exercise recommended at this stage is walking, which I usually get 30-40 minutes in per day now, broken up into two segments. This burns between 250-300 calories per day.
I am feeling very good most days. Had some bad abdominal pain that woke me up the night-before-last - was worried, but turns out it was something quite normal , likely caused by a combination of my calcium supplements and not get enough water.

Speaking of supplements, here is my regimen since surgery:
- chewable adult multi-vitamin (I will need to take this for the rest of my life)
- chewable Vitamin C and D
- Tums 2xday with food (switching to 1200 mg of Calcium Caltrate as of today)
- B12, 1 strip taken in a sublingual dissolving strip daily
- And I just started a prescription for a PPI to reduce stomach acid
 There are times when I am quite tired, though – I was not using the CPAP machine as regularly as I should have - it's been bugging me lately (Don’t you think I look like some weird Borg-Elephant hybrid when I wear it?), but I am going to give it a good try for the next month.
There are times when I am quite tired, though – I was not using the CPAP machine as regularly as I should have - it's been bugging me lately (Don’t you think I look like some weird Borg-Elephant hybrid when I wear it?), but I am going to give it a good try for the next month.
Worked two 4-hour shifts with no problem on Monday and Tuesday, but had to take the last couple of days off to deal with the abdominal pain issue. Heading back in this afternoon, because I love my job and the people there.
Working in my walks while working is going to be one my biggest challenges, I think. Just going to make sure I leave early enough so I can park my car at the Fluvarium and walk into the HSC via the Long Pond trail.
I am lucky that I got my surgery at a time when it is possible to walk outside – those of you scheduled for winter months, plan carefully!
From what I have heard, Dr. Pace is now in the process of seeing 50 other people this month to schedule them for VSG surgery sometime in the next 12 months. Surgeries will resume in July. I am so happy for those of you who are starting the journey!
We may all not be in the same boat, but we’re definitely on the same river – I’m just a little further downstream, is all, and will be waiting to cheer you on. 
Preventative Maintenance
May 30, 2011
Got my staples taken out today, blessedly, and on my way into the Major's Path clinics, I couldn't help but send up gratitude for the Canadian public health care system.
In the U.S., for instance, a VSG surgery is upwards of $12,000, no matter how medically urgent it may be. Plus, 12 grand gets you a DAY SURGERY, in and out.
By comparison, my surgery involved the input of my family physician, dieticians, a respirologist, a physiotherapist, an anaesthesiologist, three surgeons, a multitude of nurses, and follow-up a public health nurse. I stayed in hospital for three nights and I had professionals I could call or email with questions.
In short, my surgery was addressed with all due diligence and care. The health care system “invested” in my health. In return, I will be saving umpteen $$$ for our health care system in the long term by reducing my risk of a boat load of obesity-related conditions.

Dr. Laurie Twells, a researcher at Memorial University, was part of a team that did quite an interesting study into obesity in NL recently.
“The purpose of the study was to examine the association of body mass index (BMI) with the prevalence of chronic disease and health services use in adults living in Newfoundland and Labrador (NL).”
Her team had some interesting conclusions:
“In conclusion, the study findings suggest that in the NL population, increasing categories of BMI are associated with an increased likelihood of chronic diseases, especially those known to be associated with excess weight.”
“At a population level, the burden on family physicians of managing and treating obesity-associated chronic conditions is substantial. From a treatment and management perspective, more resources should be channelled into primary health care services, especially for those high-risk individuals who are morbidly obese.”
Addressing health care in a proactive sense is the only way we can preserve the magnificent benefits we enjoy in our country. Just like with a car, preserving and ensuring health is always cheaper than fixing it after it’s broke.
And I am certainly not saying that everyone who is overweight should go and get bariatric surgery. (You wouldn’t qualify, anyway.)
But for those who are morbidly obese (BMI greater than 40) AND you have extensively explored other weight loss options without long term success, thank goodness it is an option that now you can consider in our province.
The best medicine of all
May 26, 2011
A brief update about today – I feel fantastic! I read on posts on the general VSG forum that some programs prescribe B12 after surgery to help boost energy depletion from the caloric drop, so I decided to pick some B12 strips that dissolve on the tongue. It might be psychosomatic, but about 2 hours later I felt peppy for the first time since surgery! Might as well stick with it...
And now, back to the hospital:
After my delightful two-hour stay in the recovery room, they gave me what they termed a “floor dose” of morphine and off I was wheeled, bed and all up, down, around, until I heard the “Welcome to 4 North B!” and I was handed off to the unit nurse, Jamie. I had to perform a shimmy to transfer from the operating bed onto the room bed, and apparently they said that was a good sign that I could do it myself.
The rest of Friday is fuzzy, but I do remember doing a little shuffle walk down the corridor and back with one of the nurses – they REALLY want you to get up and moving as soon as possible after surgery. And since they are the ladies with the morphine, I was happy to keep them happy so they could keep me not unhappy. :)
Some of you have asked if laparoscopic surgery hurts. Hell ya! Whaddya think?
The first day the worst pain, bar none, is from the gas they insert into your abdomen during the surgery. It causes shoulder pain and stomach pain, and it really doesn’t start to clear until about 24-36 hours post-op. Suck it up and buzz every four hours for your morphine.
On the day of surgery, they wouldn’t give us anything to drink at all, so by the morning of day two, I was eager to go for my barium swallow test.
The barium swallow test is very important to check to make sure there are no leaks in the stomach after VSG surgery. Can you imagine drinking some water and having it dribble into places it’s not supposed to go?
As eager as I was, though, it was really gross. The stuff you have to drink – blech – and then stand there on this platform that jerks back and forth while they maneuver the x-ray. It was a gagsome experience, and I HIGHLY recommend asking the techs to let you suck on some ice to numb your taste buds before going for it. I didn’t do this and had to have a bucket next to me during the entire test that I could spit into.
Happily, though, the test was good and I got the all clear to go to clear liquids (water, apple juice, cran cocktail and broth – my favourite) for the next 24 hours.
The rest of the hospital stay was fairly monotonous but here are some tips and highlights:
- As soon as and whenever you get out of bed to use the bathroom, take the chance while you’re unhooked from the wall with your IV to walk the hallway. This will really speed healing and help with the gas pains.
- Don’t bring a ton of stuff to the hospital, but it was nice having my own nightshirts, robe and sandals. Plus I brought one cheerfully coloured blankie from home, which really brightened up the bed – which you will spend a lot of time in.
- Bring vaseline. Your lips get really dry in there.
- Order the television. You won’t even have the energy to read.
- You CAN bring your cell/smartphone – there is good reception and it’s cheaper than hooking up the room phone, but there is no wireless, so leave your laptop.
Initially Dr. Pace indicated that we would probably be in the hospital for two nights, but neither we, as the patients, nor the nurses felt that we were up for discharge at that time and Tracy (the other VSG patient) and I both stayed three nights.
Speaking of Tracy, I knew there was someone else slated to “get sleeved” on the same day as I was, but I didn’t know who it was. On my first night in the hospital, she stopped by my room during her first shuffle around to introduce herself and said that she already knew about me from my blog!
She had been doing some web searching about the surgery in the week prior and found my blog – how cool is that?
We spoke frequently throughout our hospital stay and will stay in touch forever, I expect – it was so awesome to have someone to share the experience with.
I think Dr. Pace will be doing surgeries in twos from here on, so definitely try and meet your surgery buddy – it was an awesome support for me.
By the time we were released on Monday, we were more than ready to go. By then I had been off of the morphine for 24 hours and was only needing to take Adasol 30’s at night and some regular Tylenol in the day.
My BFF – who had been a regular visitor throughout my stay – was there to take me home. And while I felt every bump along the way, it was so good to finally be going home.
About an hour after I arrived, my son was dropped back after spending a great weekend staying with various friends. Honestly, every time I called him from the hospital, he seemed to be having too much fun to want to stop and talk to me, so I really didn’t think he missed me that much. No odds, I was just happy he was having a good time and being so well taken care of.
So when he spent the first hour at home clinging to my neck and telling me how much he loved me, well, I think that was the best medicine of all.

No Guts, No Glory
May 25, 2011
Wow – five days post-op already. So much to update with – and a lot of it is intended for those who will be undergoing VSG themselves in the coming months, so other readers may wish to gloss over the detail of this post.
The day before surgery was only clear liquids (no biggie), and then NPO (nothing by mouth) after midnight. They also gave me a Zantac to take the night before and the morning of to recent any residual stomach acid.
I spent the evening alone after dropping my son off to my super mother-in-law for overnight, as I would have to leave early for the hospital the next morning. It was actually really good to have the time alone to go through the natural emotions you go through the night before something like this. I was able to do what I needed to do in solitude - which, for a control freak like me, included a “I hope you will never have to read this” letter of instructions in the event of the unlikely, which can now just be popped into my safety deposit box to be opened 60 years from now. :)
In any case, I actually was able to relax afterwards, read a few chapters of the latest Sookie Stackhouse novel, and get a good sleep.
The morning of my surgery, my BFF (best friend forever) picked me up bright and early at my house and drove me into the HSC, where I checked in at the surgery desk by 6:30am.
A few minutes later I was into a chair in the pre-op area undergoing prep with a very nice RN. They said that my BFF could join me in there, and since I was there over an hour, it was really nice to have the company.
First I donned a lovely green-and-blue Eastern Health ensemble,
 complete with matching booties. Then, after the pre-requisite list of the same old questions (note: many different people will ask you endlessly about you pre-existing health conditions, medications and allergies – it’s trés redundant, but just be patient, go with it and be happy there are so many checks and balances in place) I received an injection of Heperin (to prevent clotting), and doses of Maxeran (to prevent sickness) and another Zantac (stomach acid).
complete with matching booties. Then, after the pre-requisite list of the same old questions (note: many different people will ask you endlessly about you pre-existing health conditions, medications and allergies – it’s trés redundant, but just be patient, go with it and be happy there are so many checks and balances in place) I received an injection of Heperin (to prevent clotting), and doses of Maxeran (to prevent sickness) and another Zantac (stomach acid).After that, it was just a waiting game until I was called into surgery. But they gave both me and my BFF those warmed-up blankets they always seem to have on hand, so it was cozy. We did some Facebooking while we waited. ;)
Dr. Pace did stop in to see me while we were waiting, which as I understand it, surgeons don’t always do, but I wasn’t surprised, as I would be his first NL VSG patient. It was quick, but I got a chance to ask him a few questions re: swimming (2 weeks) and sex (go for it whenever I feel up to it). He also told me the team who would be in the room for my surgery:
Dr. David Pace – lead surgeon
Dr. James Ellesmere – bariatric surgeon in from Halifax to observe and assist
Dr. Darrell Boone – surgeon who is just above Dr. Pace in the food chain at Eastern Health, to observe and assist
Dr. Robert Forward – Anesthesiologist (you may remember him as Mr. 2% from my pre-admission appointment, but seriously, a great guy who makes you feel uber-groovy on the table)
Dr. Kuan Chuah – Chief surgical resident
Jill Vardy – a rep from the company that supplies the instruments for this kind of surgery
And three RN’s – Duane, Sandra, and Marilyn – sorry, I didn’t get their last names.
A few minutes later I was hugging my BFF and heading off to…another waiting room! With, you got it, another person with another list of the same questions. :)
But it was quick – more like a staging area, after which I walked with the RN into the operating theatre. (The term operating “theatre” sounds so much more comforting to me than OR, but there was really nothing very theatrical about it.)
I got up on the table and then they inserted an IV into my hand, after numbing the area a bit (thanks Dr. F!). Oxygen on the face, then the AWESOME pre-sleepy drug that kicks in like the best happy place you’ve ever been to. Hands down, the best 30 seconds of my life. :)
But it was fleeting – within moments I got delivered the good stuff and knew no more until waking up in recovery.
Now, although I don’t know what happened in the room during the surgery, I do know that there was one moment when I managed to crack the room up, even though I was unconscious.
You see, since I knew I wouldn’t have the chance to thank the team in person, this is what I left taped to my tummy for them to find before they started the surgery:


Apparently, they appreciated it a lot, which is always a nice way to start.
Recovery room was quite icky – a lot of nausea, pain, morphine, throwing up, more morphine, and a really strong-personality RN telling me to calm down and breath. She was great, actually, just what I needed. And she also held my hand, which was very comforting. I think Dr. Forward and Dr. Pace stopped in at some point, but it is an understandably fuzzy couple of hours.
I remember the first thing telling them to phone my BFF so she could phone my husband and family to let them know I was okay. I think I even managed to slur out her phone number to them, which is impressive, considering I usually need to look at a key pad to remember it! But I knew it was important for my loved ones know that I was okay. Once I knew that was taken care of, I could go back to my retching. :)
More on my hospital stay later – gotta go and see the public health nurse now to get my dressings looked at.
Later ‘gators.
Tomorrow and tomorrow and tomorrow
May 19, 2011
T-Minus 12 hours
It looks like I will be first up tomorrow, as the VSG is scheduled for 8am. They told me at the pre-admission clinic that it may take about 3 hours – no odds to me, I suppose, since I’ll be asleep – plus 60-90 minutes in recovery. Hopefully I’ll be settled into a room by lunchtime.
Yesterday was pretty interesting at pre-admission. I had to go for bloodwork, an EKG and some X-rays, and I met with an anaesthesiologist at the pre-admission clinic. He said that my EKG looked great and that I was an ideal candidate for surgery – he seemed pleased when he told me there was only a two per cent chance of fatality.
Thanks.
The pre-admission nurse was very nice and said I was down 20 pounds since I first saw Dr. Pace on March 22.
Since I had the all clear, and I knew today was an all clear liquids day – AND I had been fasting since the night before – I beat it down to India Gate with a good buddy for one last feed.
Some good.
But I can’t think about that now – today I’m starving again. Some water, a little cranberry juice and some more vile chicken broth is my sum total for today, so dwelling on butter chicken will get me no where good.
Tomorrow, after the surgery, I am going to focus on getting fluids into me – 30 cc, or about 2 tsp per hour is what I am supposed to aim for, in small sips. Hopefully by suppertime I can have some broth – my favourite, as you know. ;)
But there will be no pity – only joy and gratitude. Joy that tomorrow will mark a super-step in my journey back to health, and gratitude for all of the wonderful Canadian health care resources and personnel who are making it possible.
Yes, I am a little scared. But I am DOING this. Everything I believe about why still holds true.
And here are my two most important reasons of all.

Thanks for the love. Talk to you on the flipside.
The Road to Referral
May 16, 2011
T-minus 4 days
In my first post I alluded to a story behind my referral to bariatric surgery. I am a little amazed by it, and hope that those of you who have been on a wait list for a long while will forgive the hand of fate that is behind my own story.
There have been many times in the last few years that I have thought about how the “weight issue” was starting to impact my health and I began discussing it as “the root of all evil” with my family physician. I had her start monitoring my weight, so that I would have some extra accountability when I went through various diet and exercise stages.
Then my body started sabotaging my attempts at exercise – ankles and knees didn’t hold up like they used to, and I had increasing trips to the massage therapist and chiropractor.
Diets worked for a while, but it seemed I would always find some reason to backslide – I was too busy, I was on vacation, it was a special occasion, even just that it was really damn cold and my body craved comfort food.
Last fall, in one of my bluer days, I asked my doctor whether or not she thought bariatric surgery was a viable option for me. To be honest, I kind of expected her to say no, that it was an extreme option only for patients much bigger than me.
To my surprise, she said that it can be sometimes the only long-term solution for many, many patients, and she felt that if it was an option I wanted to pursue, she would be behind me 100%.
(This is probably a good time for me to tell the world how awesome my doctor, Dr. Marie O’Dea, is, and always has been – a good doctor is a gift from God.)
So that was all I need to send me scurrying off to the Internet in my research. My earliest searches led me to this web site that hosts my blog, from which I have learned so much from so many.
The first thing I learned is that bariatric surgery is either a) a long wait, b) expensive, or c) both. Plus, at the time, there was no one in Newfoundland performing any type of bariatric surgery, so I would have to travel out of province for both pre-op appointments and the surgery itself.
There are three types of bariatric surgery that are the most common in Canada; the Roux-n-Y Gastric Bypass; the Gastric Lap Band; and the Sleeve Gastrectomy (which I have discussed at length in other posts)
Gastric bypass surgery is the most common and makes the stomach smaller and allows food to bypass part of the small intestine. It is not reversible. This surgery is covered by MCP and was the likeliest option for me initially. I knew that there were surgeons in many others provinces who performed this.
The gastric lap band is an inflatable banding system that is placed around the upper stomach to limit food intake. It can be adjusted, depending on the needs of individual patients, and is reversible. At the time I inquired (fall 2010), it was not covered by MCP. I inquired at several facilities in the Toronto area, and the cost was approximately $16,000. The good news was that the procedure could have been performed within 6-10 weeks from first referral.
Not having $16,000 lying around, I decided to ask Dr. O’Dea for a referral for gastric bypass. She also referred me for approval by MCP for an out of province procedure, which I also received. (MCP would pay for medical costs, but not for any travel, which was okay.)
The next step was finding a surgeon. While I knew that most patients in NL were referred to New Brunswick, first I tried to find a surgeon in Ontario that would accept me, as my family is in Toronto. Ontario boosted its bariatric surgery program with seventy-five (75) million dollars in 2009, so I thought they would have plenty of surgeons.
Oh, they do – just not a single one willing to take anyone from out-of-province. The obesity “epidemic” is so high in Ontario that despite my elegantly-phrased appeals to several surgeons, they were unable to accept anyone out-of-province and despite their program boost, most surgeons still had an 18-month to 2 year wait list.
Meanwhile, the waitlist for a New Brunswick surgeon was reported to be in the 5-7 year range. No matter, I said to myself, just start the first step and I’ll wait my turn.
Then – the hand of fate intervened. A colleague of mine mentioned the possibility of a bariatric program starting in Newfoundland under Dr. David Pace. Before you could say wham-bam-thank you ma’am, I had my referral into his office.
My referral appointment was March 22, and all I hoped for at that stage was that he would accept me into his program. I was so joyful at the possibility of getting the surgery at home; I didn’t care how long I would have to wait.
Now I know surgeons are not often known for their bedside manner, but when he said he would be scheduling me for the first day of surgery in May, I could have kissed him!
So, dear friends and fellow bariatric-surgery hopefuls, indeed, I have a horseshoe up my bum and (dare I say it?) a guardian angel by my side. I am LUCKY and BLESSED to be getting this surgery on Friday, which will be approximately seven months since I began looking into it.
I know many of you have been waiting much longer than I have, and I am so sorry for that. I will pray for your success in equal measure to my hoped-for own.
